BlueSpeak Newsletter
April 2026 BlueSpeak
Welcome to the April 2026 BlueSpeak Provider Newsletter. If you have questions about these updates, call the Blue KC Provider Hotline at 816-395-3929 for our Commercial line of business or 866-859-3822 for the Affordable Care Act (ACA) Provider Hotline. Thank you for your partnership in providing quality care to our members.
Additional audit requirements for $1M claims
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
- 1 ACA QHP: Affordable Care Act Qualified Health Plan for Individual/Family
- 2 JAA: Joint Administrative Account
- 3 FEP: Federal Employee Program
- 4 Medicare Advantage (BlueCard): Medicare Advantage for other Blue Cross Blue Shield Association plans
Effective July 1, 2026, Blue Cross and Blue Shield of Kansas City (Blue KC) is adding steps to our in-depth prepay review on any claim that will allow $1M or more. To ensure Blue KC can continue to perform this prepay review, medical records and/or itemized bills will be required for these claims.
Billing updates
Updated notice: Billing change for implanted prosthetic device
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
- Effective June 1, 2026, coverage for C1776 will be limited to one (1) unit per surgical encounter.
- The code applies only to the implanted prosthetic device used during joint replacement procedures (e.g., knee, hip, shoulder).
- As an update to the March 2026 BlueSpeak Newsletter, anchors and screws for bone fixation or for opposing bone-to-bone or soft tissue to bone may be reported separately with C1713 and C1741.
- The device must be billed on the same claim as the corresponding surgical procedure.
- If an encounter requires more than one unit, medical records must be submitted to support medical necessity for review and determination.
- Documentation must clearly support the implanted joint device consistent with CMS and Coding Clinic guidance.
Prior Authorization Updates
Code addition
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
The following codes will be added to our prior authorization list, effective June 1, 2026.
| Code | Description | Effective Date | Lines of Business Impacted |
| 0019M | Cardiovascular disease, plasma, analysis of protein biomarkers by aptamer-based microarray and algorithm reported as 4-year likelihood of coronary event in high-risk populations | 6/1/2026 | Commercial, ACA |
Medical Policy Updates
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
The most up-to-date Medical Policy can be found by logging into Providers.BlueKC.com and clicking on the Medical Policies section. While on that web page, you can also find a link to view Milliman Care Guidelines (MCG), which complement our Blue KC policies.
The Blue KC Medical Policy encompasses internal Blue KC Medical Policy, Blue Cross Blue Shield Association derived Medical Policy, and policies adopted from our vendor partners, such as Avalon, MCG and eviCore.
Note: This is not a comprehensive list of updates.
| Effective date – 5/1/2026 |
ID: AHS-M2145 Title: General Genetic Testing Germline Disorders – Avalon Update
|
| Effective date – 5/1/2026 |
ID: AHS-M2114 Title: Pancreatic Cancer Risk Testing Using Pancreatic Cyst Fluid – Avalon Update
|
| Effective date – 5/1/2026 |
ID: AHS-M2176 Title: Testing for Developmental Delay – Avalon Update
|
Pharmacy Policy Updates
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
Below are new Blue KC pharmacy policies effective May 1, 2026, for medications that already require prior authorization. Note: This is not a comprehensive list of updates.
| New Pharmacy Policies | ||
| Policy Number | Policy Name | Summary |
| 5.02.587 | Blenrep (belantamab mafodotinblmf) | FDA Approved for Relapsed or refractory (R/R) multiple myeloma (MM); IV; Medical-Rx benefit |
| 5.02.695 | Reinduction Dosing Requests for Biologics | Requests for reinduction dosing regimen may be medically necessary for the following reasons: 1) loss of therapeutic response after initial induction, 2) interruption of therapy due to clinical events, 3) adverse events leading to temporary discontinuation, 4) pharmacokinetic considerations |
Below are Blue KC pharmacy policies with updates effective May 1, 2026, for medications that already require prior authorization. Note: This is not a comprehensive list of updates.
| Pharmacy Policies with Changes | ||
| Policy Number | Policy Name | Summary |
| 5.02.676 | Ziihera (zanidatamab-hrii) | Removed step through Enhertu |
| 5.02.636 | Lunsumio (mosunetuzumab) | Updated criteria to add: 1) Patient is 18 years of age or older, 2) The patient has not had prior treatment with chimeric antigen receptor T-cell (CAR-T) therapy within 30 days before administration of Lunsumio, 3) The patient has not had an allogeneic hematopoietic stem cell transplant, 4) The patient has not had an autologous stem cel transplant within the past 100 days, 5) The patient has no history of CNS lymphoma or CNS disorders, 6) The patient has no active infection (e.g. viral, bacterial, fungal) such as HIV, active hepatitis B or active hepatitis C, 7) The patient has received 2 or more prior lines of therapy that includes anti-CD20 therapy (e.g., rituximab) and an alkylating agent (e.g., cyclophosphamide) |
Payment Policy Updates
To find the complete version of Blue KC Payment Policies, click here or go to the login page at Providers.BlueKC.com and click on “Go to Payment Policies”, which lists All Provider Payment and Coding Policies and Lab Payment Policies. Note: This is not a comprehensive list of updates.
| Payment Policies Featured in this Section |
| Hemodialysis, Home Hemodialysis and Peritoneal Dialysis Services |
| Chiropractic and Osteopathic Manipulative Services |
Hemodialysis, Home Hemodialysis and Peritoneal Dialysis Services Payment Policy
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
| Policy Number | Policy Name | Enforcement Date | Full Policy Location |
| POL-PP-233 | Hemodialysis, Home Hemodialysis and Peritoneal Dialysis Services | 7/1/2026 |
View our Hemodialysis, Home Hemodialysis and Peritoneal Dialysis Services Payment Policy Visit our Payment Policies page Go to Providers.BlueKC.com, click on “Go to Payment Policies” |
Reminder
- As a reminder, POL-PP-233 Hemodialysis, Home Hemodialysis and Peritoneal Dialysis Services Payment Policy requires that procedure code is billed with the most recent Urea Reduction Ratio (URR) for the dialysis patient. URR modifier goes with Code 90999.
- Beginning July 1, 2026, facility claims billed with a missing, incorrect or invalid modifier will be denied, and a corrected claim will need to be resubmitted with the appropriate modifier to be considered for payment.
-
Urea Reduction Ratio: All hemodialysis claims must indicate the most recent Urea Reduction Ratio (URR) for the dialysis patient. If the modifier is not present, the claim will be denied and returned for the appropriate modifier.
- G1 Most recent URR of less than 60%
- G2 Most recent URR of 60% to 64.9%
- G3 Most recent URR of 65% to 69.9%
- G4 Most recent URR of 70% to 74.9%
- G5 Most recent URR of 75% or greater
- G6 ESRD patient for whom less than seven dialysis sessions have been provided in a month
Chiropractic and Osteopathic Manipulative Services Payment Policy
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
| Policy Number | Policy Name | Full Policy Location |
| POL-PP-212 | Chiropractic and Osteopathic Manipulative Services |
View our Chiropractic and Osteopathic Manipulative Services Payment Policy Visit our Payment Policies page Go to Providers.BlueKC.com, click on “Go to Payment Policies” |
Reminder
- As a reminder, per our Chiropractic and Osteopathic Manipulative Services Payment Policy update in 2024, Blue KC implemented an edit that the number of spinal areas manipulated needed a separate diagnosis to support each area. Last year, Blue KC made an enhancement on that edit that included diagnosis pointers. The number of diagnoses must support the number of spinal areas manipulated. Below is additional information from the policy to help providers bill correctly.
-
Spinal Manipulative Procedures
- Chiropractic manipulative treatment (CMT) CPT codes 98940- 98942 are used to indicate the number of spinal areas manipulated.
- The problem/complaint addressed, and precise level of each subluxation treated, must be specified in the medical record.
-
The level of the subluxation must be specified on the claim and must be listed as the primary diagnosis.
- Example
- 98942 – Chiropractic manipulative treatment (CMT); spinal, 5 regions. Diagnosis should be specific to the location of the subluxation. CPT 98942 represents 5 different spinal regions; there must be a subluxation diagnosis to support each region.
- Areas of treatment should be documented separately in spinal regions (e.g., cervical, thoracic, lumbar, sacrum and pelvic) and vertebral (C1-S5).
- When billing, if providers are using the terms “all spinal regions”, “upper and lower spinal regions” and “all affected regions”, these terms do not support the service performed to the degree of specificity required.
Provider Education
Interpreter services from Blue KC
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
Blue KC wants providers to know that we offer interpreter services to your patients in every language.
Below is information about the linguistic needs and preferences of the people in our communities and how you can access language services for your patients.
-
Here is a look at some of the data from the top 15 languages spoken by individuals in the Kansas City metro, according to recent statistics from the U.S. Census Bureau’s sample of five percent of the population.
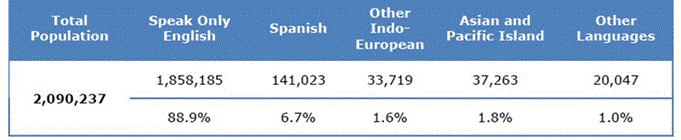
-
Did you know interpreter services are available?
- If you are seeing a Blue KC Member and would like interpretation services to help that member in any language, call 1-844-395-7126.
- If someone you are helping has questions about Blue KC, they have the right to get help and information in their language at no cost. In addition to talking to an interpreter in any language, they can visit https://www.BlueKC.com/non-discrimination-information/.
-
Did you know training is available on the provision of language services?
- The Joint Commission and Department of Health & Human Services offer the following free training: Physicians - Think Cultural Health.
Tips for Independent Laboratory Claims
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
Blue KC wants to inform providers that we are seeing an increase in clinical edit denials on independent laboratory claims. Blue KC is providing the information below to help resolve this issue for all providers who utilize independent laboratory vendors for testing.
| Why is Blue KC seeing an increase in clinical edit denials on independent laboratory claims? |
|
| What policy do providers need to follow? |
|
| For more information |
|
Free documentation & coding webinar in May
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
Join us for the May monthly webinar hosted by our partner, Veradigm! This is a free documentation and coding education webinar. Each 1-hour webinar is approved for one AAPC CEU when you achieve a 70% or higher on the post-test. To register for the webinar, click here for details:
|
May 26 & 28 |
Documentation Matters: |
Build a strong foundation in risk adjustment by learning the essentials of thorough documentation for accurate coding. |
A better GAP fill schedule
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
Blue KC is pleased to have recently improved the format of the GAP Fill Fee Schedule, which you can access by logging into Providers.BlueKC.com and selecting the GAP Fill Fee Schedule tab under Resources. Here are some of the recent improvements we made following your feedback:
- Added a column to designate Facility or Non-Facility allowable pricing.
- When the file is downloaded, the effective date is now reflected in the file name.
New Provider Portal login page
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
Have you noticed our new-look Blue KC Provider Portal login page at Providers.BlueKC.com?
Blue KC is making it easier for you to get the information you need by providing additional quick access link options that take you directly to the section of the portal you are interested in seeing.
Here’s how this new section appears on the login page:
Make sure to log in to take advantage of all the Blue KC Provider Portal functions, including submitting a new or viewing an existing prior authorization and our provider data forms. Here are some helpful forms on our Portal:
-
General Inquiry Form
- For a faster way to answer your questions.
-
Provider Updates Form
- For updates in between initial credentialing and re-credentialing cycles
-
Initial Credentialing Forms
- For solo/rendering practitioners and ancillary/facility providers new to Blue KC.
- Revalidation Credentialing Forms
For non-contracted provider groups, ancillaries and facilities interested in joining Blue KC’s networks, select ““Join Blue KC Networks” on our login page at Providers.BlueKC.com.
For claims related inquiries, please use the Claim Inquiry Form (Providers.BlueKC.com/eForms/Form/ClaimInquiry), which provides the following category options:
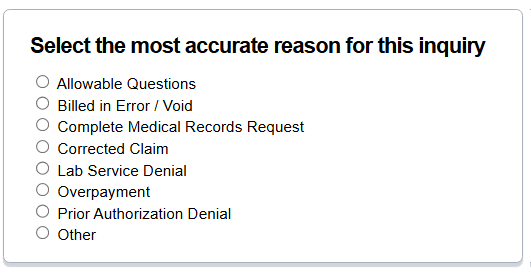
You are also able to use this Claim Inquiry form to request the status of a previous inquiry if a response has not been received within 30 days.
Recently enhanced Blue KC Provider Reference Guide now available
| LINE OF BUSINESS IMPACTED | ||||||
| COMMERCIAL | ACA QHP1 | SMALL GROUP ACA | JAA2 | FEP3 | Medicare Advantage (BlueCard)4 | Dental |
| The BLUE highlighted box is the line of business impacted by this update. | ||||||
|
|
|
|
Community Investment
Giving Back: Blue KC Volunteers Plant Orchard at DeLaSalle Learning Farm

On April 16, more than 40 Blue KC volunteers joined nearly 100 high school students at DeLaSalle Education Center at 37th and Troost in Kansas City, Mo. to help plant an orchard, as part of the school’s Learning Farm initiative.
The Learning Farm will provide free access to healthy food to help DeLaSalle become a new center for urban agriculture.
Blue KC, along with behavioral and mental health nonprofit Cornerstones of Care, its vocational program Build Trybe, The Giving Grove and Kansas City Community Gardens planted 20 fruit trees, that included apple, pear, peach, pecan and cherry trees.
The orchard will have the ability to produce almost 4,700 pounds of food annually with the potential to produce 103,000 pounds of food over its lifetime, all to help provide free access to healthy food for the school and surrounding community.
Healthy Kids Day: Blue KC Supports YMCA of Greater Kansas City

On April 18, more than 2,000 families participated in Healthy Kids Day, presented by Blue Cross and Blue Shield of Kansas City, at the North Kansas City YMCA.
Kids participated in sports clinics, STEAM activities and free wellness, dental and vision screenings, while attendees made non-perishable food donations to support YMCA food pantries.
Contact Us
Please join the BlueSpeak email distribution list by sending a request to BlueSpeak@BlueKC.com. You can also use this email address to give us any feedback about BlueSpeak. We would love to hear from you!
If you have questions about any of these updates, please call the Blue KC Provider Hotline at 816-395-3929 for Commercial line of business or 866-859-3822 for the ACA Provider Hotline. We value and appreciate you as our partner in providing quality care.
An independent licensee of the Blue Cross and Blue Shield Association
© Blue Cross and Blue Shield of Kansas City. All rights reserved.